A father recounts his emotional journey caring for his toddler son who is a “butterfly” child.

“My son Aryan, now 4, was born in March 2015 in a Singapore private hospital. The day after he was born, the nurse came around to give him the usual round of vaccinations. I noticed small blisters forming on his butt but the nurse assured me that these blisters were normal for newborns and there was no need to worry. The doctor also prescribed cream and advised me to apply it on the blisters and it would gradually subside.
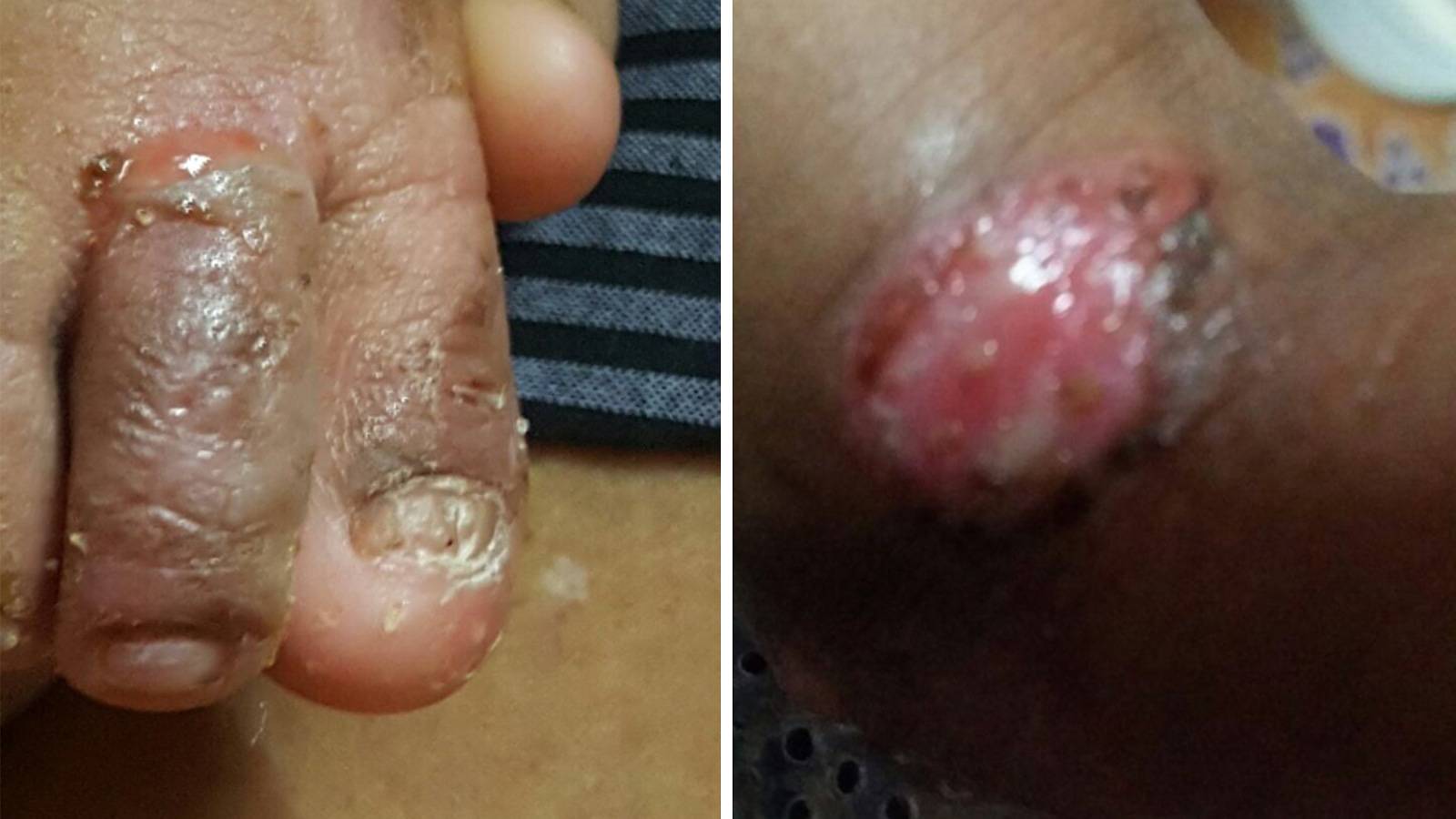
By the third day when we were home, I started seeing blisters forming on Aryan’s foot and some on the fingers of his left hand. Puzzled and worried that these would spread further, my wife Divya and I decided it would be best to see the doctor. Before our visit, I managed to speak to him on the phone. He reassured me that the blisters were probably due to the heat and we should observe him for a few days before deciding what to do. It didn’t take that long for us to notice that something was amiss.
Over the course of the next few hours, we began to see new blisters forming in different parts of Aryan’s body — they seemed to be ‘moving’ to more areas. What was worse, the earlier blisters also grew bigger. The cream given by the doctor had no effect at all ― I wanted to poke the blisters to clear the fluid but Divya told me not to.
“I learnt later that with Aryan’s condition, bandaging the wounds together can actually cause the fingers to fuse together.”
When we didn’t see any improvement in Aryan’s condition that night, we decided to head for the hospital, thinking the doctor who delivered my son should know more about the condition. On the way to the hospital, one of the blisters on Aryan’s foot grew so big, it burst. On using a cloth to absorb the fluid, I saw that the skin on the sole of his foot was open and raw.
When we arrived at the hospital at 2am, we were told that they don’t operate an emergency department, so we had to wait till morning to see the doctor. So for six long hours, Aryan cried through the night as my wife and I tried to do whatever we could to comfort him.
Finally, when we saw the doctor at 8am, he took samples of the fluid from Aryan’s blisters and admitted him. Every evening for the next four days, Aryan received antibiotics through an IV drip. The nurses also dressed Aryan’s wounds in paraffin wax gauze and bandages, and also bandaged his fingers in a long piece of gauze. I learnt later that with Aryan’s condition, bandaging the wounds together could actually cause the fingers to fuse together.
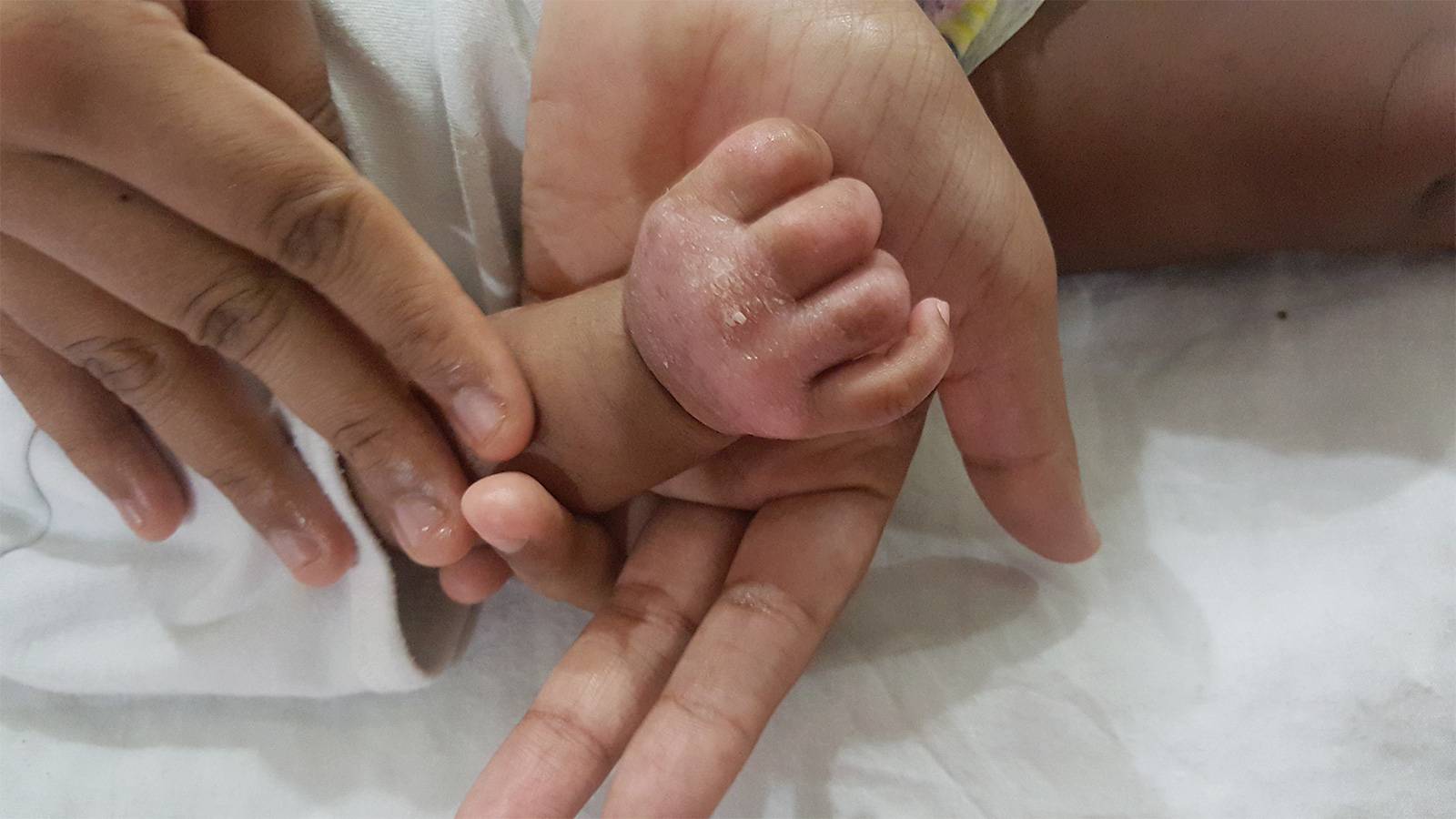
After four days, there was no improvement at all in Aryan’s condition. My wife and I were in a state of despair, feeling as if we’d lost our son. On the fourth day, the dermatologist came and upon reviewing Aryan’s records, told us that our son has Epidermolysis Bullosa (EB). It is a condition where any skin contact can cause it to blister, resulting in open wounds and sores. Aryan suffers from a cross between simplex and dystrophic types of EB (see below).
We decided it was best to take Aryan to the emergency department at KK Women’s and Children’s Hospital. The doctor on duty referred us to Dr Mark Koh — medical advisor to DEBRA Singapore, a support group for caregivers or patients with EB. Although we were relieved at first to hear of a specialist who could attend to Aryan, we soon found out that we had to wait six months for the earliest appointment! I pleaded with the doctor because my son couldn’t possibly wait six months to see Dr Koh!
Life with EB
After a quick phone call, Dr Koh came around and brought the three of us to his lab where he took samples from us for testing. I asked him if Aryan could stay in his lab until he was cured of EB. To my shock, Dr Koh told me that there’s no medication available for Aryan — EB is a lifelong condition for which there is no cure.
He says from now on, we just need to know how to properly dress Aryan’s wounds and once he is of age, he can learn how to do it on his own.
The first two to three months of caring for Aryan were tough as we don’t have help at home. But my wife was great throughout this trying time. She took Aryan’s diagnosis in her stride and went online to do her research like watching YouTube videos on alternative care techniques.
“If we don’t clear up the blisters quickly, there’s a chance it would grow to about the size of a one dollar coin.”
It has become routine to do a full body check on our son every morning, then every two hours. If we don’t clear up the blisters quickly, there’s a chance it would grow to about the size of a one dollar coin. If the blister is located on his arms or legs, Aryan won’t feel them as much. But it can be very painful on sensitive spots like the sole of his foot or the palms of his hands. So, we only poke these blisters when he’s asleep so that we won’t disturb him.
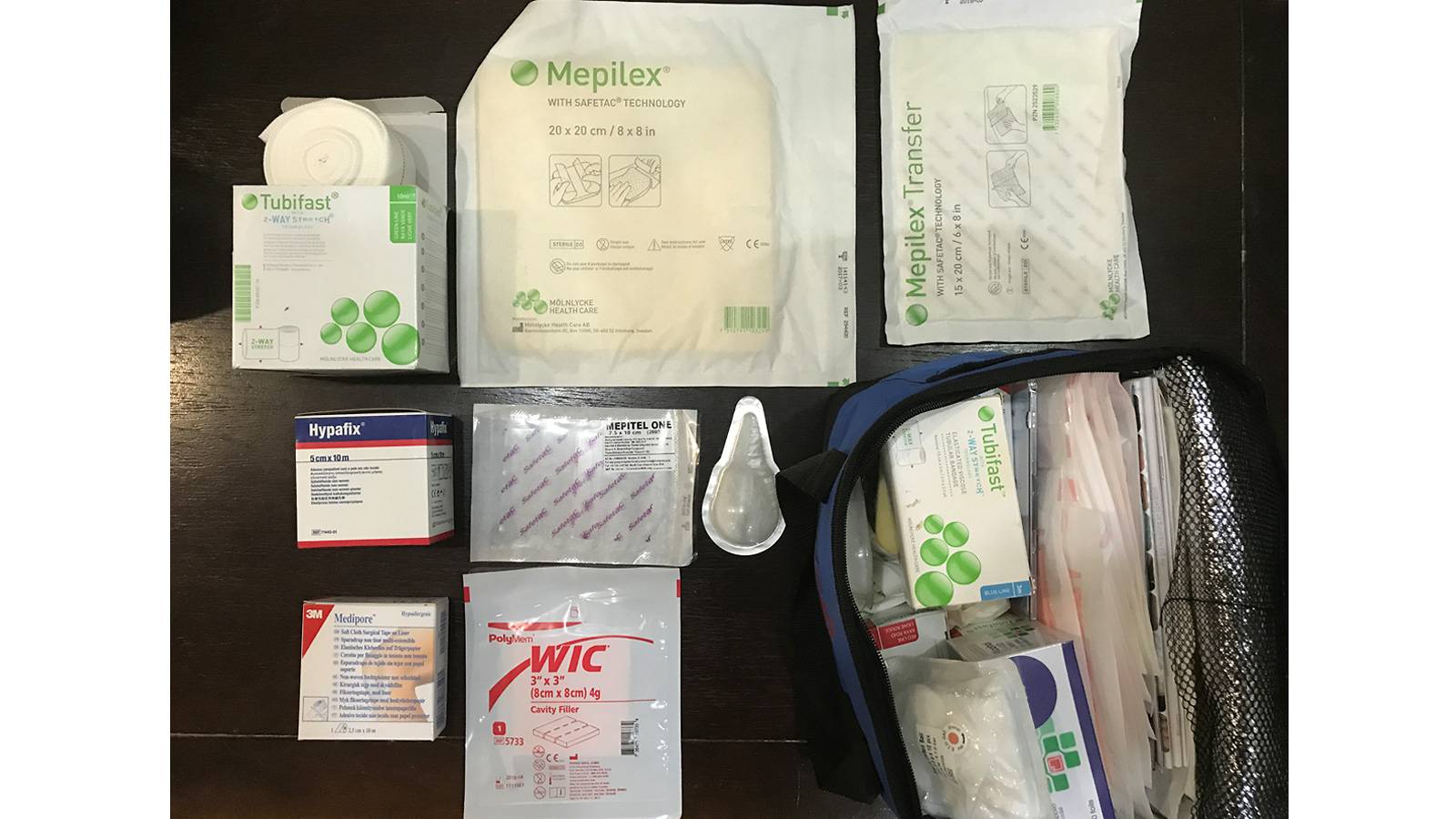
The bandages we use to dress Aryan’s wounds aren’t the usual ones you buy off the shelves — it contains polymer, which prevents it from sticking to the skin. A strip measuring 10cm to 18cm costs $15 and can only last two days. We also need to use special gels. Just our medical supplies alone can cost about $200 to $300 — sometimes, $400 ― a month.
This amount can be a considerable financial strain ― since my son is on a long-term visa, I can’t make any CPF claims. But the funds we’re getting from DEBRA Singapore make the costs a little more manageable.
Dr Koh also advises us to keep Aryan’s skin cool, to minimise irritating the skin, which is why I need to keep the air-conditioner running all day. We have little choice as the afternoon heat can cause his soles to develop blisters. That’s why we also dress him in clothes made of bamboo fibre — it is softer to the touch and also aids in cooling the skin.
When your child has a delicate skin condition, you realise there are many things they can’t do, not without hurting themselves accidentally. Even normal developmental changes like crawling can result in blisters because of the contact between the knees and the ground. Luckily, Aryan didn’t crawl at all — he learnt to flip over and sit up straight instead.
As for bathing, you may not realise this, but our chlorinated tap water causes Aryan pain whenever we bathe him ― there are occasions when he’ll end up in tears. We also have to avoid hot water at all costs as the heat can trigger blisters. Divya and I will pour the warm water on our skin to test if it is okay before pouring it on him.
Whenever we are out, only my wife and I can carry Aryan. If someone else carries him, I will need to check the other person’s clothes or accessories to prevent Aryan’s skin from getting caught or suffering abrasions.
Now that he is 2, we need to pay even more attention to him because he is super-active — running and walking everywhere. When I run with him, I have to be mindful not to reach out suddenly and grab him. If I do, I risk creating more wounds, which has happened before.
“When I run with him, I have to be mindful not to reach out suddenly and grab him. If I do, I risk creating more wounds, which has happened before.”
Despite these challenges, I’m very grateful that my family won’t need to face EB alone — I have a group of DEBRA Singapore parents in whom I can count on. I’ve gained a wealth of knowledge and tips from other parents who are confronting the same — if not more daunting — set of challenges.
I’ll be the happiest man in the world if a cure for Aryan’s condition is found. I’m not hoping that my son will become a doctor or hold down some prestigious job in the future. So long as he’s able to grow up and be able to interact confidently with others and know about the world around him, I’m happy.”
Dhanasekar Sampath, 36, and married to Divya Parasuraman, 28, live with their son Aryan, 4, in the western part of Singapore.

What is EB?
Dr Mark Koh, DEBRA Singapore’s medical advisor, notes that about three to five children are born with Epidermolysis Bullosa (EB) in Singapore each year. Explains Dr Koh, who also heads the dermatology service at KK Women’s and Children’s Hospital, “Although usually an inherited genetic condition, EB can [also] occur for the first time in certain families.”
Children with EB are often referred to as the “butterfly children” as their skin is as fragile as the wings of a butterfly — it blisters and tears from minor skin contact with anything. In some cases, the condition can be lethal before the age of 30. People with EB, the two skin layers ― the epidermis and dermis ― lack the protein “basement” anchors that hold them together.
While there are five types of EB — simplex, dystrophic junctional, kindler syndrome and aquisita ― these are the three most common ones:
*Simplex EB Blisters are formed on the hands, feet or all over the body. With good wound and pain management, many simplex EB sufferers are able to lead fulfilling lives.
*Dystrophic EB These sufferers usually display fused fingers and toes and a narrowing of the oesophagus. Patients also face an increased risk of developing squamous cell carcinoma, an aggressive form of skin cancer, before the age of 35.
*Junctional EB is a far more severe and rare form of EB — occurring in just five per cent of EB cases in the US. The symptoms include extensive blistering all over one’s body, markings or skin damage particularly on the face. Worse, blisters can also form on the inside of one’s oral tracts like the pharynx and oesophagus. Children with severe forms of Junctional EB usually die within the first two years of their life from malnutrition and anaemia.
How you can help
Your financial assistance can benefit families like Dhanasekar’s in defraying the financial cost of caring for their EB children. A donation to DEBRA Singapore will also fund research as well as efforts to increase public awareness of the devastating condition. Find out more here.
Photos: Dhanasekar Sampath
Also check out other dramatic true stories here.
Like us on Facebook and check SmartParents regularly for the latest reads!
Elsewhere on SmartParents.sg…
6 things you didn’t know about eczema